"Curse of knowledge" leading to health information difficult for readers - 2026
Research published in Patient Education and Counselling, says health information remains stubbornly difficult for patients to understand—not because experts lack effort, but because of a deeper cognitive trap known as the “curse of knowledge.”
Once professionals gain expertise, they lose the ability to see information from a layman’s perspective, leading them to unintentionally use jargon, skip essential steps, and overload readers with detail.
This matters far beyond communication: when people can’t clearly understand information about conditions, treatments, or prevention, it directly limits their ability to make informed decisions and to look after their own health with confidence.
Researchers say governments failing to implement physical activity policy - 2026
Policies encouraging physical activity have failed to make a tangible difference, according to researchers.
The authors of a study in Nature Health called for more coordinated action across different sectors such as transport, housing, and education to reverse this trend.
They said physical activity should not only be promoted for its benefits in tackling cardiovascular disease, but acknowledged for its contribution to other goals such as improved mental health and climate resilience.
Five million deaths a year are attributed to physical inactivity globally.
Vitamin D levels in your 30s might shapen your brain in later years - 2026
People with higher vitamin D levels in early midlife are more likely to have lower levels of tau protein in their brains years later — and tau is one of the key proteins associated with Alzheimer’s disease. Findings are from a study with 800 people with an average age of 39, none of whom had dementia. All participants had vitamin D measured at the start; brain scans followed 16 years later. The lead researcher noted that midlife is a time where risk factor modification can have a greater impact.
You might be ageing faster because of difficult people in your life - 2026
Published in the Proceedings of the National Academy of Sciences, a study looked at “hasslers” – people in your close social network who regularly make life harder. Each additional hassler is associated with faster biological ageing. Effects are particularly pronounced when the hassler is a family member.
Your morning coffee might be protecting your brain - 2026
A study of more than 130,000 people which followed them for 43 years found that moderate consumption of caffeinated coffee or tea was linked to an 18% lower risk of developing dementia, with the benefits appearing strongest at 2-3 cups of coffee or 1-2 cups of tea daily.
Decaffeinated coffee showed no such benefit, suggesting caffeine itself, together with polyphenols, plays a significant role.
Alcohol use linked to heart disease and stroke - 2025
A scientific statement from the American Heart Association examined research connecting alcohol use with heart disease and stroke. Some studies suggested low to moderate alcohol intake may be beneficial, although more recent research challenged this notion. Evidence clearly linked heavy alcohol use (3 or 4 drinks daily) to the risk of elevated hypertension, stroke, heart failure and atrial fibrillation.
The study underscores the need for more rigorous randomised controlled trials to better understand alcohol’s true impact on cardiovascular health. It also emphasises the importance of prioritising well-established lifestyle practises like regular physical activity and a balanced diet to prevent heart disease.
Healthy eating in midlife helps us age well - 2025
Research from Harvard, the University of Copenhagen, and the University of Montreal found that diets rich in plant-based foods and low in ultra-processed foods are linked to healthier ageing. The study followed over 105,000 participants, aged 39 to 69, for 30 years. Those who followed healthier diets, like the Alternative Healthy Eating Index (AHEI), had better chances of ageing well. Participants in the top AHEI group were 86% more likely to age healthfully at 70 and 2.2 times more likely at 75. The research suggests that a plant-based diet with moderate healthy animal foods can support healthy ageing..
Microplastics linked to chronic disease like diabetes, stroke and high blood pressure- 2025
Research from Case Western Reserve School of Medicine, shows that tiny plastic particles, called microplastics, may be linked to serious health problems like high blood pressure, diabetes, and stroke. Microplastics are commonly found in the environment, including in food, beverages, and air. The study found that areas with higher levels of microplastics in water also had higher rates of these diseases. More research is needed to prove that microplastics directly cause health issues. In the meantime, researchers recommend reducing plastic use and improving waste disposal to help lower microplastic pollution. Taking care of the environment might also help protect our health.
5 minutes of daily exercise can significantly improve physical and mental health - 2025
A study by Edith Cowan University found that just five minutes of daily eccentric exercise can significantly improve physical and mental health in sedentary individuals. The home-based program, which included bodyweight exercises like chair squats and wall push-ups, focused on slow, muscle-lengthening movements. Participants saw improvements in muscle strength, flexibility, endurance, and mental well-being. The research suggests that even small, accessible exercises can offer sustainable benefits without the need for a gym.
Morning coffee may protect the heart better than all-day coffee drinking - 2025
Research by the European Heart Journal has found that it’s not the amount of coffee we drink that protects against heart disease and stroke but the time we drink it. Comparing morning coffee drinkers with all-day coffee drinkers and non-coffee drinkers, the study found that morning drinkers who drank 2-3 cups each day had a lower risk of dying from a heart attack or stroke by a third compared to those in the other categories. Researchers are unsure why but believes it could be due to it not interfering with circadian rhythms in the body.
Self-Care Observatory - 2025
The Self-Care Observatory features papers curated by international experts, including both authoritative sources and grey literature, with an initial focus on making 10 high-quality papers per subject readily accessible. The platform allows for the growth of its repository while prioritising accessibility to important research.
The collection is freely available to anyone interested in self-care, as well as those who want to help others take better care of their health, supported by evidence-based research.
Knowledge is Power survey by PIF and IPSOS - 2024
Adults in the UK are increasingly struggling to find reliable health information, with clear inequalities in access to trustworthy resources, “Knowledge is Power”, a new report from the Patient Information Forum (PIF) and Ipsos, sheds light on the challenges surrounding information access, trusted sources, communication with healthcare professionals, and the growing impact of misinformation.
The report is based on a nationally-representative survey of 2,003 adults across the UK conducted from May to June 2024 using the Ipsos KnowledgePanel. It highlights the strong public demand for the NHS to guide individuals to trustworthy information.
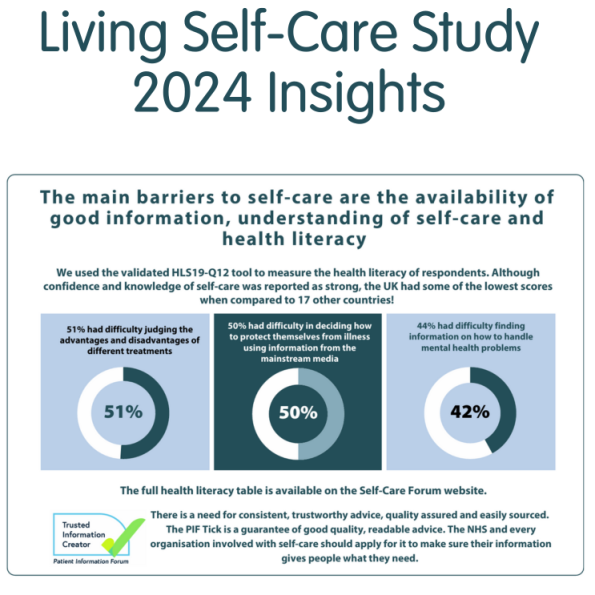
Self-Care Forum self-care behaviour and attitudes interim results- 2024
An early deep dive into self-care research by the Self-Care Forum and Imperial College London’s SCARU (Self-Care Academic Research Unit) reveals one of the major barriers to people taking better care of their own health is the lack of consistent, clear, and understandable health information. Lead author Dr Peter Smith OBE, Self-Care Forum President, concludes that such information is essential throughout life, starting at school age.
Called the Living Self-Care Survey, research sought to investigate public and health professional knowledge, attitudes and behaviours to self-care in the UK found that most people self-cared when they have symptoms, with 49 per cent taking OTC medication, 42 per cent doing nothing and 4 per cent consulting their GP.
The NHS: Is it still there for us when we need it? - 2024
Research by the Policy Institute at King’s College London, King’s Business School and Ipsos found that belief that the NHS will be there for people when they need it has fallen considerably over the last 16 year in the UK.
Between 2008 and 2024 the share of Britons who agreed with this view declined from 82% to 66%. Around 1 in 5 (18%) people now feel the NHS won’t be there for them when they need it, double the 9% who held this view in 2008.
50% of the British population say they had a health condition in the last 12 months that they thought of contacting their GP practice about but didn’t.
Early findings from NHS T2 diabetes programme - 2024
Research shows that one-third of participants with type 2 diabetes who complete the NHS England Type 2 Diabetes Path to Remission programme, which includes the ‘soups and shakes’ diet, achieve remission.
The findings, published in The Lancet Diabetes & Endocrinology, cover the period from September 2020 to the end of 2022. During this time, 7,540 people were referred to the programme.
Of these, 1,740 participants began the ‘soups and shakes’ diet before January 2022, and 945 completed the year-long programme. The results revealed that 32% of those who completed the programme put their type 2 diabetes into remission, with an average weight loss of 16kg.
Smoking Trends Among Women Under 45 in England: A Decade-Long Study - 2024
According to a study conducted by researchers at University College London (UCL) and funded by Cancer Research UK, there has been an increase in smoking among women under 45 from more advantaged social groups in England over the past decade.
It found the percentage of women in the more advantaged social groups (ages 18 to 45) who smoked rose from 12% to 15% between 2013 and 2023.
In contrast, less advantaged women of the same age group saw their smoking rates decline steadily during the same period, from 29% to 22%.
Among adults overall, smoking declined over the 10-year period, although this decline flattened during the pandemic.
Education key to enabling self-care - 2023
Research by the consumer health association, PAGB confirms that education is key to increasing self-care with 4 in 5 (83 per cent) of those surveyed saying we need more education to encourage people to take a more proactive approach.
The research also found that 2 in 5 adults (39 per cent) requested a GP appointment for common health conditions including colds, a blocked nose, insect bites and stings and headaches; with 8 per cent of people visiting A&E for conditions such as dandruff, acne, head lice and other non-urgent and relatively minor health conditions.
11 minutes of brisk walking sufficient to lower risk of disease such as heart disease, stroke and some cancers - 2023
One in ten early deaths could be prevented if everyone managed at least half the *recommended level of physical activity, say a team led by researchers at the University of Cambridge.
In the study which was published in the British Journal of Sports Medicine, the researchers say that 11 minutes a day (75 minutes a week) of moderate-intensity physical activity – such as a brisk walk – would be sufficient to lower the risk of diseases such as heart disease, stroke and a number of cancers.
*The NHS recommends 150 minutes of moderate intensity activity, or 75 minutes of vigorous activity a week.
8,000 steps a day can reduce the risk of premature death - 2023
An international study led by the University of Granada has identified for the first time the optimal number of steps at which most people obtain the greatest benefits, and also shows that the pace at which you walk provides additional benefits.
The idea that you should take 10,000 steps a day originated in Japan in the 1960s, but had no scientific basis. Researchers have now shown that, if we focus on the risk of dying from cardiovascular disease, most of the benefits are seen at around 7,000 steps with 8,000 expressed as the optimal range.
Any activity is better for your heart than sitting - even sleeping - 2023
Replacing sitting with as little as a few minutes of moderate exercise a day tangibly improves heart health, according to new research by University College London. Supported by the British Heart Foundation, this is the first study to assess how different movement patterns throughout the day are linked to heart health.
The study found that while small changes can have a positive effect on heart health, intensity of movement also matters.
How has COVID-19 changed healthcare professionals’ attitudes to self-care? - 2023
This research studied the views of a cross-section of the healthcare workforce following the COVID-19 pandemic to understand if service users, who largely practised self-care during the pandemic, would continue these practices as a first option after the pandemic.
Self-Medication in Europe: Economic and Social Impact on Individuals and Society - 2023
National healthcare systems across Europe are facing financial and recruitment challenges. With this in mind, researchers sought to examine the economic and social value of self-medication in Europe. They found that there is already value associated with self-medication but that this can be increased further by promoting self-care. Resources freed-up through an adequate self-care policy can play a significant role in building more resilient health systems across Europe, researchers found.
Soups and Shakes helped people with T2 Diabetes go into remission - 2023
Losing weight can put type 2 diabetes in remission for at least 5 years, new data has suggested.
Figures from the Diabetes Remission Clinical Trial (DiRECT) show that around a quarter of people in remission from diabetes 2 years after starting a low-calorie “soup and shakes” diet were still in remission 3 years later.
These people no longer needed to take medication to manage their blood sugar levels and had an average weight loss of around 1st 6lb (8.9kg) at the 5-year point.
The data suggests that losing weight and keeping it off can help reverse diabetes.
Has the pandemic changed self-care attitudes? - 2023
A research study by Self-Care Forum President, Dr Pete Smith and Trustee, Dr Austen El Osta sought to understand how self-reported professional attitudes, perceptions and practices of self care changed as a result of the COVID-19 pandemic.
Respondents, made up of pharmacists, nurses, GPs, social prescribers and other health and social care professionals, said the importance of self-care had increased markedly during the pandemic. Indeed, respondents who felt self-care was extremely important to their service-users increased from 54 per cent to 86 per cent.

Vaping e-cigarettes as harmful for your lungs as smoking cigarettes - 2023
A research paper, published in The Journal of Nuclear Medicine, warned that vaping can “cause pulmonary inflammation and increases the risk of lung disease”. The research suggests that e-cigarette users have greater lung inflammation than cigarette smokers. This study is the first to provide evidence that vaping e-liquids with e-cigarettes creates a unique inflammatory response in the lungs that is different from cigarette smoking.
Walking towards healthier knees - 2022
A study reveals that walking for exercise can reduce new frequent knee pain among people aged 50 and older diagnosed with knee osteoarthritis, the most common form of arthritis. Additionally, findings from the study indicate that walking for exercise may be an effective treatment to slow the damage that occurs within the joint.
Heavy drinkers four times more likely to smoke in England, study finds - 2022
Research by the University of London found that those who are among the heaviest drinkers in England are four times more likely to smoke than the general population. Because of the findings, experts say heavy drinkers should be prioritized by the government in its plans to achieve ‘smoke-free’ status by 2030.

Walking at pace may help to slow down the biological ageing process - 2022
University of Leicester research of 400,000 UK adults found a link between walking pace and a genetic marker of biological age, estimating that a lifetime of brisk walking could lead to the equivalent of 16 years younger biological age by midlife.
While the physical, mental, social and health benefits of walking are well-documented, this study is one of the first of its kind to compare genetic data with both self-reported walking speeds, as well as actual measurements of movement intensity from wearable activity tracking devices worn by participants.

One-minute bursts of activity during daily tasks could prolong your life - 2022
In good news for those who don’t like playing sport or going to the gym, research finds just three to four one-minute bursts of huffing and puffing during daily tasks is associated with large reductions in the risk of premature death, particularly from cardiovascular disease.
This study, by the University of Sydney’s Charles Perkins Centre in Australia, is the first to accurately measure the health benefits of what researchers have termed ‘vigorous intermittent lifestyle physical activity’ or VILPA.
Higher rate of hip fractures amongst vegetarian women - 2022
A Leeds University study of more than 26,000 middle-aged UK women reveals those with a vegetarian diet had a 33% higher risk of hip fracture compared to regular meat-eaters.
The research, published in BMC Medicine, investigated the risk of hip fracture in occasional meat-eaters, pescatarians (people who eat fish but not meat) and vegetarians – compared with regular meat-eaters.
Among 26,318 women, 822 hip fracture cases were observed over 20 years (3% of the sample population). After adjustment for factors such as smoking and age, vegetarians were the only diet group with an elevated risk of hip fracture.
Education, job, and social life may help protect the brain from cognitive decline - 2022
A study explored the possibility that a healthy social and working life, and education, could help us ward off cognitive decline in our brain.
Some people with amyloid plaques in their brains associated with Alzheimer’s disease show no signs of the disease, while others with the same amount of plaque have clear memory and thinking problems.
UK researchers looked at genetic and life course factors that may help create a “cognitive reserve” that provides a buffer against the disease.
They found that taking part in clubs, religious groups, sports or artistic activities, occupation and reading ability, may affect the brain’s cognitive reserve.
Chronic pain in England: Unseen, unequal and unfair - 2021
This report, produced by Versus Arthritis, uses data from the Health Survey for England 2017 to improve our understanding of chronic pain in our society. We know this is a huge problem – a third of people aged 16 years and over reported living with chronic pain, and just over one in ten people report that they
are struggling to cope with severe chronic pain, known as high-impact chronic pain. The majority of people with chronic pain have musculoskeletal conditions like arthritis, although chronic pain is also linked to other health conditions. Versus Arthritis is calling for chronic pain to be viewed as a public health problem requiring a public health solution.

Developing, piloting and evaluating a Medicines Safety School Programme to be delivered by student pharmacists - 2021
This project aimed to develop content, pilot delivery, and evaluate effectiveness of an innovative Medicines Safety School Programme delivered by student pharmacists to primary school pupils.
The Medicines Safety School Programme has been well received by the pupils, school staff, and student pharmacists involved in the pilot study. Development of the programme is ongoing and is now progressing to embed this innovative educational initiative into the pharmacy undergraduate curriculum.
The Cost of Inequality - putting a price on health - 2021
This paper by the Centre for the Study of Financial Innovation proposes a novel way of thinking about inequalities, linking health to wealth and to the economy.
It shows, for example, that a one-year extension in healthy life expectancy would add around 3.4 months to working lives and 4.5 months to overall life expectancy. It also shows that it is generally more efficient to focus policy on increasing healthy life expectancy than on extending the total life span.
Fruit, veg and exercise can make us happier - 2021
Research by the University of Kent and University of Reading found that eating fruit and vegetables, as well as exercising can increase levels of happiness.
While the link between lifestyle and wellbeing has been previously documented and often used to encourage healthier lifestyle habits, findings published by the Journal of Happiness Studies show that there is also a positive causation from lifestyle to life satisfaction.
This research is the first of its kind to unravel the causation of how happiness, the consumption of fruit and vegetables and exercising are related, rather than generalising a correlation.
Self-Care Vital to Healthy Ageing – 2021
The World Economic Forum, says human lifespan really does have a limit though self care is vital to healthy ageing. Research which looked at the “invariant rate of ageing” found that humans have a built in tendency to age.
Though life expectancy has risen since the mid-1800s due to healthier, safer societies we will not live forever because ageing is built into our genes. Scientists believe the “absolute limit” is 150 years but, one thing is clear, however long we live, self care is vital to healthy ageing. So, stick to a healthy diet, keep active, drink only in moderation, don’t smoke and you could live to be 150.
Limit TV Watching to 2 hours says researchers – 2020
According to a study by scientists at Glasgow University restricting TV watching time for adults could increase longevity. Analysis of information from 500,000 Britons aged from 37 to 73 over seven years showed that 6 per cent of all-deaths and 8 per cent of cardiovascular related deaths could be associated with too much TV watching. The study findings pointed to too much time spent watching TV resulting in less exercise and poor diet.
Food Supplements can help brain development – 2020
Dr. Me. “significantly improves” schoolchildren’s self care knowledge – 2020
A study of more than 200 schoolchildren showed that Dr. Me. – a self care presentation designed by GP Dr Chee Yeen to empower schoolchildren – was shown to significantly improve their understanding of how to self care minor conditions.
The children attended workshops covering vomiting and diarrhoea; sore throat and fever; and minor head injuries. In the study, six case scenarios were asked at the beginning and end of the session, and children decided whether to stay home, visit the GP or attend A&E.
Living longer but not necessarily healthier: The joint progress of health and mortality in the working-age population of England – 2020
According to research in Population Studies – A journal of demography, we are living longer but not necessarily in good health.
The study which looked at generational health, suggests that younger generations can no longer expect to lead healthier lives than their ancestors. People in England in their forties and fifties are, on average, in significantly worse physical shape than those now in their sixties and seventies were at the same age.
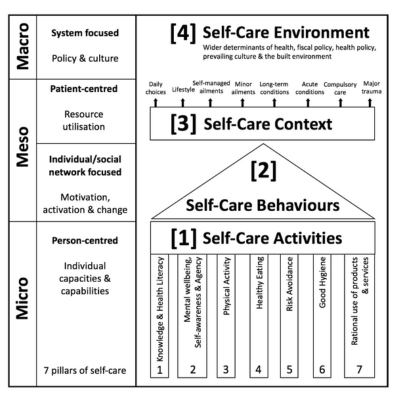
The self-care matrix: a unifying self-care framework – 2019
This article was published in the Self-care Journal following a review of academic and lay literature to identify conceptual models of self-care; devising a matrix to be used to view, identify, study and evaluate self-care elements in any health and wellbeing intervention, independent of the disease category or setting.

A natural approach to health works – 2019
Leeds Beckett University undertook a social return on investment analysis of Wildlife Trust Programmes and found that targeted programmes designed for people with a health or social need showed a return of £6.88 for every £1 invested. This value was generated from health gains such as improved mental wellbeing. The research showed a range of benefits, such as increased feelings of positivity and levels of physical activity.
Reducing antibiotic prescribing for self-limiting respiratory tract infections in primary care – A pilot study by Dr Pete Smith et al 2015
Churchill Medical Centre, a primary care centre in Surrey, implemented a practice-wide programme aimed at patients and clinicians to reduce ineffective antibiotic prescriptions for common respiratory tract infections.
The evidence for investing in high quality health information for patients and the public – 2013
The Patient Information Forum (PiF) commissioned research to identify the benefits of investing in health information. The project found that there are good reasons to justify the investment in health information provision and support. These include positive impacts on service use and costs, substantial capacity savings, and significant returns on investment by increasing shared decision-making, self-care and the self-management of long-term conditions.
Primary Care: Today and Tomorrow – Improving general practice by working differently –2012
According to this report, general practices need to develop ways of working with patients to help them improve their health rather than simply treating their “episodic illness”. Improved information and communications in practices is needed, developing shared decision-making and self care strategies to help educate patients into taking care of their own health.
Helping People Help Themselves – 2011
The Health Foundation has produced this literature review to respond to the questions and challenges of clinicians wanting to appraise the benefits of self-management support.
This review of more than 550 pieces of high quality research suggests that it is worthwhile to support self-management, in particular through focusing on behaviour change and supporting self-efficacy.
Self Care Aware: Joining up Self Care in the NHS – 2007
JUSC is a strategy to improve the interface between primary care and the community. This will ensure that service demand is efficiently managed, actively supporting the individual’s own ability to combine self care, when possible, with primary care, when needed.
A Picture of Health – 2005
A national consumer survey into people’s experience of everyday ailments and health conditions such as colds, headaches, allergies, indigestion and muscle aches, and how they deal with them.
The findings offer a fascinating insight into how we manage our everyday health and in particular our preference for looking after ourselves as far as we can.